Coronary Heart Disease
 |
| Click Image to Enlarge |
What are the coronary arteries?
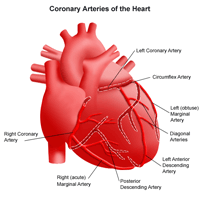
Coronary arteries supply blood to the heart muscle. Like all other tissues in the body, the heart muscle needs oxygen-rich blood to function, and oxygen-depleted blood must be carried away. The coronary arteries consist of two main arteries: the right and left coronary arteries. The left coronary artery system branches into the circumflex artery and the left anterior descending artery.
What are the different coronary arteries?
The two main coronary arteries are the left and right coronary arteries. The left coronary artery (LCA) divides into the left anterior descending artery and the circumflex branch. The left anterior descending artery supplies blood to the front of the left side of the heart and the circumflex artery supplies blood to the lateral side and back of the heart. The right coronary artery (RCA), which divides into the right posterior descending and acute marginal arteries, supplies blood to the right ventricle, right atrium, and sinoatrial node (cluster of cells in the right atrial wall that regulates the heart's rhythmic rate), and atrioventricular node (AV node, a cluster of cells between the atria and ventricles that regulate the electrical current).
Smaller branches of the coronary arteries include: acute marginal, posterior descending (PDA), obtuse marginal (OM), septal perforator, and diagonals.
Why are the coronary arteries important?
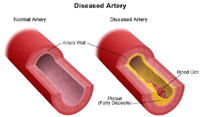
Since coronary arteries deliver blood to the heart muscle, any coronary artery disorder or disease can have serious implications by reducing the flow of oxygen and nutrients to the heart, which may lead to a heart attack and possibly death. Atherosclerosis (a build-up of plaque in the inner lining of an artery causing it to narrow or become blocked) is the most common cause of heart disease.
 |
| Click Image to Enlarge |
What is coronary artery disease?
Coronary artery disease (CAD) is characterized by the accumulation of fatty deposits along the innermost layer of the coronary arteries. The fatty deposits may develop in childhood and continue to thicken and enlarge throughout the life span. This thickening, called atherosclerosis, narrows the arteries and can decrease or block the flow of blood to the heart.
Nearly 13 million Americans suffer from coronary artery disease - the number one killer of both men and women in the US.
What are the risk factors for coronary artery disease?
Risk factors for CAD often include:
-
high LDL cholesterol, high triglycerides levels and reduced HDL cholesterol
-
high blood pressure (hypertension)
-
physical inactivity
-
smoking
-
obesity
-
high saturated fat diet
-
diabetes
-
age
-
family history
-
excessive alcohol intake
Controlling risk factors is the key to preventing illness and death from CAD.
What are the symptoms of coronary artery disease?
The symptoms of coronary heart disease will depend on the severity of the disease. Some persons with CAD have no symptoms, some have episodes of mild chest pain or angina, and some have more severe chest pain.
If too little oxygenated blood reaches the heart, a person will experience chest pain called angina. When the blood supply is completely cut off, the result is a heart attack, and the heart muscle begins to die. Some persons may have a heart attack and never recognize the symptoms. This is called a "silent" heart attack.
When symptoms are present, each person may experience them differently. Symptoms of coronary artery disease may include:
-
heaviness, tightness, pressure, and/or pain in the chest - behind the breastbone
-
pain radiating in the arms, shoulders, jaw, neck, and/or back
-
shortness of breath
-
weakness and fatigue
-
rarely, abdominal pain and indigestion-like symptoms
How is coronary artery disease diagnosed?
In addition to a complete medical history and physical examination, diagnostic procedures for coronary artery disease may include any, or a combination of, the following:
-
electrocardiogram (ECG or EKG) - a test that records the electrical activity of the heart, shows abnormal rhythms (arrhythmias or dysrhythmias), and detects heart muscle damage.
-
stress test (usually with ECG; also called treadmill or exercise ECG) - a test that is given while a patient walks on a treadmill to monitor the heart during exercise. Breathing and blood pressure are also monitored. A stress test may be used to detect coronary artery disease, and/or to determine safe levels of exercise following a heart attack or heart surgery.
-
cardiac catheterization - with this procedure, x-rays are taken after a contrast agent is injected into an artery - to locate the narrowing, occlusions, and other abnormalities of specific arteries.
-
nuclear scanning - radioactive material is injected into a vein and then is observed using a special camera as it is taken up by the heart muscle. This shows the healthy and damaged areas of the heart.
-
echocardiogram - an ultrasound of the heart that measures the pumping function of the heart (also known as ejection fraction or EF) and assesses the function of the heart valves and muscle walls.
Treatment for coronary heart disease:
Specific treatment will be determined by your physician based on:
-
your age, overall health, and medical history
-
extent of the disease
-
your tolerance for specific medications, procedures, or therapies
-
expectations for the course of the disease
-
your opinion or preference
Treatment may include:
-
modification of risk factors - Risk factors that may be modified include smoking, elevated cholesterol levels, elevated blood glucose levels, lack of exercise, poor dietary habits, and elevated blood pressure.
-
medications - Medications that may be used to treat coronary artery disease include:
-
antiplatelet medications - medications used to decrease the ability of platelets in the blood to stick together and cause clots. Aspirin, clopidogrel (Plavix®), ticlopidine (Ticlid®), and dipyridamole (Persantine®) are examples of antiplatelet medications.
-
anticoagulants - also described as "blood thinners," these medications work differently than antiplatelet medications to decrease the ability of the blood to clot. An example of an anticoagulant is warfarin (Coumadin®).
-
antihyperlipidemics - medications used to lower lipids (fats) in the blood, particularly Low Density Lipoprotein (LDL) cholesterol. Statins are a group of antihyperlipidemic medications, and bile acid sequestrants - colesevelam, cholestyramine and colestipol - and nicotinic acid (niacin) are two other types of medications that may be used to reduce cholesterol levels.
-
antihypertensives - medications used to lower blood pressure. There are several different groups of medications which act in different ways to lower blood pressure
-
drugs that relieve angina - nitroglycerin
-
drugs that regulate heart rate and blood pressure - beta blockers
-
drugs that improve heart function - ACE inhibitors
To make an appointment in the Cardiovascular Medicine Division at BWH call: 617-732-4837.
-
catheter-based treatment/coronary angioplasty - with this procedure, a catheter is used to create an opening in the blocked vessel to increase blood flow. Although angioplasty is performed in other blood vessels, Percutaneous Transluminal Coronary Angioplasty (PTCA) refers to angioplasty in the coronary arteries to permit more blood flow into the heart. There are several types of PTCA procedures, including:
-
balloon angioplasty - a small balloon is inflated inside the blocked artery to open the blocked area.
-
coronary artery stent - a tiny coil is expanded inside the blocked artery after balloon angioplasty to keep the artery open.
-
bare metal stent - a tiny metal coil which is placed in the artery and is incorporated by the body into the wall of the coronary artery over a period of a few months.
-
drug eluting stent- a bare metal stent covered with a medication that prevents renarrowing (or "restenosis") at the site of stent treatment, which can occur in up to 20% of patients treated with bare metal stents. The drug eluting stents are extremely effective in reducing the chance or renarrowing at the site of stent placement, but require that patients remain on aspirin and Plavix® or other anti-platelet medication to prevent any blood clots from forming in the coronary stent.
-
atherectomy - the blocked area inside the artery is cut away by a tiny device on the end of a catheter.
To make an appointment in the Interventional Cardiology Service (Cardiac Catheterization) at BWH call: 617-732-7133.
Cardiac Surgical Treatments
-
coronary artery bypass - Most commonly referred to as simply "bypass surgery". This surgery is often performed in people who have angina (chest pain) and coronary artery disease (where plaque has built up in the arteries). During the surgery, a bypass is created by grafting a piece of a vein above and below the blocked area of a coronary artery, enabling blood to flow around the obstruction. Veins are usually taken from the leg, but arteries from the chest and forearm may also be used to create a bypass graft. Traditionally, this operation is performed with the heart stopped and the use of a heart-lung machine.
-
off-pump CABG - In this operation, the bypasses are performed with the heart beating and without the use of a heart-lung machine. We reserve this operation for selected patients, generally those with severe co-morbid medical conditions including advanced lung disease, borderline kidney function, critical carotid artery disease, or severe atherosclerosis of the ascending aorta.
-
transmyocardial revascularization (TMR) - This is a procedure reserved for patients with critical coronary artery disease and crippling angina who are not candidates for bypass surgery or stents. TMR uses laser to "shoot" 20-45 small, pencil-lead sized "channels" in the heart muscle. It is based on the principle that, although these channels quickly close up on the outside, they remain open on the inside of the heart creating, in essence, new vessels for blood to flow through freely. These new channels could supply the heart with oxygen and nutrients. TMR may not be suitable for and benefit all patients equally. BWH cardiac surgeons have been national leaders in clinical use of this advanced technique for patients with severe coronary artery disease who are not candidates for more conventional therapies.
-
coronary endarterectomy - BWH surgeons have gained national prominence in this exclusive technique for patients with diffuse coronary artery disease. Here, the core of cholesterol material is stripped from the inner walls of the coronary arteries and the arteries are then reconstructed to allow free flow of blood. It carries higher than usual risk.
To make an appointment in the Cardiac Surgery Division at BWH call: 617-732-7678.
-
Hybrid Approach to Treatment of Coronary Artery Disease - Development of new technology has allowed for a combination of therapies to be delivered to a single patient in order to optimize outcome and reduce operative morbidity. With the advent of the more refined stents in the interventional cardiology field and the development of surgical robotics, patients may be able to receive both catheter-based and surgical therapies for coronary artery disease. Currently, surgical robotics allows for off-pump single or double vessel bypass from the side of the chest without having to split the breast bone down the middle. The same patient can have the remainder of their coronary artery disease treated by catheter-based stents, either at the same sitting or perioperatively. Not all patients will be candidates for this approach since the individual patient characteristics will determine candidacy.
To make an appointment, call either the Cardiac Surgery Division at 617-732-7678 or the Interventional Cardiology Service (Cardiac Catheterization) at 617-732-7133.
Click here to view theOnline Resources of Cardiovascular Disease